Introduction
Among patients with End-Stage Renal Disease (ESRD), Peritoneal Dialysis (PD) rather than Hemodialysis (HD) represents a treatment option which may confer temporary survival benefits, lower cost, and potentially higher patient satisfaction, but has also been associated with higher failure rates [1]. Regardless of dialysis type, patients with ESRD are known to experience higher rates of perioperative morbidity than those with normal renal function due to infectious and cardiac complications [2]. Perioperative management of PD remains controversial due to limited data and concerns about its potential surgical complications.
Specific perioperative considerations relate to the known risk of dialysis catheter leakage, which can increase the risk for peritonitis, and catheter occlusion or failure. Historically and in the general surgery literature, general principles of perioperative management have included temporary transition to HD, with consideration of low-volume peritoneal dialysis at the time of resumption of PD to decrease the likelihood of catheter leakage following re-initiation due to increased intraabdominal pressure [3-6].
Few reports exist in the literature of perioperative management of peritoneal dialysis among patients undergoing hysterectomy. While data from general surgery may be extrapolated to gynecologic laparoscopy, hysterectomy presents a unique challenge due to the dependent location of the vaginal cuff. The present case demonstrates perioperative management of a patient on PD undergoing hysterectomy through temporary conversion to HD with plans to resume PD postoperatively.
Case report
Patient history, clinical findings, and medical interventions
A 47-year-old woman, para 3, with a known history of abnormal uterine bleeding, presented to the emergency department with acute on chronic vaginal bleeding. Her medical history included end-stage renal disease secondary to type 2 diabetes mellitus, congestive heart failure, hypothyroidism, and class II obesity with BMI 38. She was on peritoneal dialysis for her end-stage renal disease. Surgical history was notable for 3 prior Cesarean deliveries, with tubal ligation procedure performed at the time of her last Cesarean delivery. On presentation, she reported 5 days of abnormal uterine bleeding and was found to have hemoglobin level of 5.0 g/dL.
The patient’s abnormal uterine bleeding was suspected to be secondary to adenomyosis versus ovulatory dysfunction, exacerbated by platelet dysfunction from her renal disease. Her bleeding was refractory to multiple medical and procedural treatments, and she had several prior emergency department presentations with acute on chronic anemia requiring blood transfusions. She had failed prior management with oral medroxyprogesterone acetate, dilation and curettage procedure, levonorgestrel intrauterine device placement, leuprolide injection, oral norethindrone, and uterine artery embolization. Prior workup was notable for benign endometrial pathology on biopsy, and pelvic ultrasound showed uterine size 11.6 × 6.0 × 5.7 cm with mildly heterogeneous myometrium which was noted to be nonspecific but consistent with adenomyosis. Given she continued to have severe abnormal uterine bleeding requiring multiple blood transfusions, recommendation was made to proceed with definitive surgical management via hysterectomy. She received a total of 5 units of packed red blood cells during her admission to achieve a hemoglobin level of 9.2 g/dL prior to undergoing hysterectomy.
Regarding her end-stage renal disease, she had been started on peritoneal dialysis therapy just over two years prior to presentation. She had regular follow-up with nephrology as an outpatient and was performing home peritoneal dialysis six times per week. On presentation, she had a creatinine elevation to 13.55 mg/dL from her baseline of 9 mg/dL. Given her acute on chronic abnormal uterine bleeding as well as multiple medical comorbidities, she was admitted to the inpatient gynecology service for surgical optimization until she would be able to undergo hysterectomy. Nephrology was consulted and recommended transition to Hemodialysis (HD) for the perioperative period. A tunneled dialysis catheter was placed by the interventional radiology team without complication and the patient underwent hemodialysis the night prior to her surgery.
Surgical management
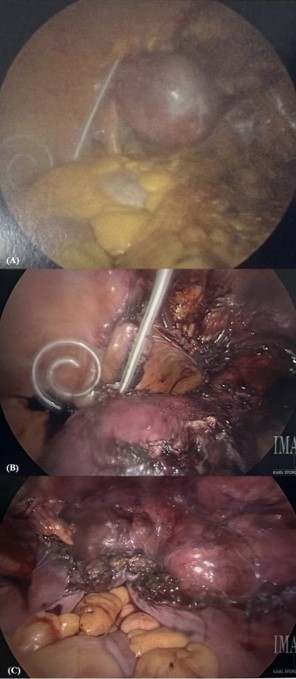
The patient underwent exam under anesthesia, laparoscopic lysis of adhesions, total laparoscopic hysterectomy, and cystoscopy. The peritoneal dialysis catheter was located in the patient’s left lower quadrant and was prepared in the sterile fashion using chlorhexidine and remained on the surgical field. Upon entry, abdominal survey was notable for scarred white peritoneum and dense omental adhesions to the anterior abdominal wall in the area of her prior Cesarean incision and adjacent to the peritoneal dialysis catheter (Figure 1A & 1B). Adhesiolysis was performed without complication and the hysterectomy was otherwise completed without issue, with estimated blood loss of 100 mL, and final pathology showing a 238 g uterus with extensive adenomyosis and focal degenerative change. The vaginal cuff was closed laparoscopically with care to incorporate the peritoneum, as the plan was to eventually restart peritoneal dialysis, and laparoscopic port sites were closed in usual fashion (Figure 1C).
Follow-up
Postoperatively, the patient did well. Labs from the post-anesthesia care unit were notable for potassium of 5.9 mmol/L, which resolved with insulin, dextrose-containing intravenous fluids, and bumetanide. She resumed hemodialysis on postoperative day 1 in the hospital and was discharged home without complication on postoperative day 2. She was advised to continue hemodialysis for 2 weeks postoperatively, while flushing her peritoneal dialysis catheter once per week, after which she could resume peritoneal dialysis.
At her 4-week postoperative appointment, the patient was healing well from a surgical perspective but had not yet resumed PD. When an attempt was made to transition the patient from HD back to PD, her PD catheter was noted to be occluded and was therefore unable to be used. The patient continued with HD three times per week until she was able to have her PD catheter replaced 4 months postoperatively, delayed secondary to logistical/nonmedical indications.
Discussion/conclusion
This case of a 47-year-old woman with ESRD undergoing total laparoscopic hysterectomy demonstrates an attempt at management of PD through temporary conversion to HD. The patient had an initially uncomplicated postoperative course. Unfortunately, when reconversion from HD to PD was attempted four weeks postoperatively, the PD catheter was noted to be occluded and required replacement.
Few cases have previously been reported on perioperative management of PD among patients undergoing hysterectomy. Most of these reports demonstrate management through temporary conversion to HD, with varying degrees of success. In a 2017 report, Kakuda and colleagues describe a total laparoscopic hysterectomy performed in a patient with a history of renal transplant [7]. The patient was converted to HD in the perioperative period, however postoperative resumption of PD was unsuccessful due to persistent leakage of dialysis fluid from the area around the catheter. This occurred despite the use of suture and fibrin glue at trocar insertion sites and closure of peritoneum. A similar technique is outlined in a 2018 case report by Ueda and colleagues, with the patient successfully transitioning back to PD on postoperative day 16 [8].
An alternative technique is demonstrated in a 2016 report by Lew and colleagues, in which a patient undergoing hysterectomy was successfully transitioned to frequent low-volume PD exchanges in supine position starting on postoperative day 3 [9]. While this technique was effective in preventing metabolic or wound complications, it required prolonged bed rest in the supine position, and postoperative course was complicated by opiate-associated constipation and peritonitis requiring intraperitoneal antibiotics. Minimal data exists to discuss supracervical hysterectomy as an option to decrease the risk of complications related to the dependent nature of the vaginal cuff and to obviate the need for prolonged supine positioning.
The ideal perioperative management of peritoneal dialysis among patients undergoing laparoscopic hysterectomy remains controversial, and few reports exist to help guide management. The present case demonstrates a valuable example of temporary conversion to hemodialysis, complicated by occlusion of the PD catheter which ultimately required replacement. Hysterectomy presents the unique challenge of operating in the area directly adjacent to the PD catheter, and suture lines in the dependent portion of the pelvis, which may be more susceptible to increased intraabdominal pressures with dialysis. Further study is merited to determine the optimal perioperative management of PD for patients with ESRD undergoing total laparoscopic hysterectomy.
Declarations
Conflicts of interest: The authors have no conflicts of interest relevant to this article.
Funding: This research did not receive any external funding.
References
- Sinnakirouchenan R, Holley JL. Peritoneal Dialysis Versus Hemodialysis: Risks, Benefits, and Access Issues. Adv Chronic Kidney Dis. 2011; 18: 428-432.
- Palamuthusingam D, Nadarajah A, Johnson DW, Pascoe EM, Hawley CM, Fahim M. Morbidity after elective surgery in patients on chronic dialysis: a systematic review and meta-analysis.
- Auricchio S, Mari G, Galassi A, et al. Laparoscopic Left Hemicolectomy for Colon Cancer in Peritoneal Dialysis Patients: A Valid and Safe Surgical Technique to Ensure Peritoneal Dialysis Survival. Perit Dial Int. 2016; 36: 695.
- Leblanc M, Ouimet D, Pichette V. Dialysate Leaks in Peritoneal Dialysis. doi:10.1046/j.1525-139x.2001.00014.x
- Mari G, Scanziani R, Auricchio S, Crippa J, Maggioni D. Laparoscopic Surgery in Patients on Peritoneal Dialysis: A Review of the Literature. 2017; 24: 397-401.
- Lew SQ. Peritoneal Dialysis Immediately after Abdominal Surgery. 2018; 38: 5-8.
- Kakuda M, Kobayashi E, Tanaka Y, Ueda Y, Yoshino K, Kimura T. Total laparoscopic hysterectomy for endometrial cancer in a renal transplantation patient receiving peritoneal dialysis: Case report and literature review. J Obstet Gynaecol Res. 2017; 43: 1232-1237.
- Ueda S, Tanaka T, Miyamoto S, Terai Y, Ohmichi M. Total Laparoscopic Hysterectomy for Adenomyosis in a Patient Receiving Peritoneal Dialysis: A Case Report. Integr Gynecol Obstet J. 2018; 1.
- Lew SQ, Chernofsky MR. Uninterrupted Peritoneal Dialysis after Robotic-Assisted Total Laparoscopic Hysterectomy. Perit Dial Int. 2016; 36: 349.